Claim denials don’t just delay payments—they expose weaknesses in the revenue cycle that, if left unaddressed, continue to repeat. As medical billing becomes more data-driven, we’ve seen how relying on instinct or manual reviews alone is no longer enough. By applying claim denial analytics, we’re able to uncover denial pattern trends that reveal why claims are denied and, more importantly, how we can stop them from happening again. At Pro MD Medical Billing, we use analytics-based denial prevention to help healthcare providers fix denial issues at the root—not just resubmit claims after the fact.
Understanding Claim Denial Analytics
Claim denial analytics focuses on analyzing denial data collectively instead of reviewing claims one by one. When we look at denial data in isolation, patterns are easy to miss. However, when we apply structured analytics, trends quickly emerge that point to systemic issues within coding, documentation, or front-end processes.
At Pro MD Medical Billing, we use claim denial analytics to turn raw denial data into actionable insights. This allows us to move from reactive billing corrections to proactive denial prevention strategies that protect revenue over the long term.
The Importance of Data Patterns
Data patterns provide invaluable insights into claim denials. By analyzing these patterns, we can identify trends and anomalies that might be contributing to the problem. For instance, a sudden increase in denials related to coding errors could indicate a need for additional training or system updates.
- Identify Frequent Issues: By recognizing patterns, we can pinpoint recurring issues that lead to denials.
- Enhance Efficiency: Understanding these patterns allows us to streamline the claims process, reducing the time and resources spent on rework.
- Implement Preventive Measures: Data patterns help in devising strategies to prevent future denials, thus improving the overall revenue cycle.
Denial Pattern Trends and Their Implications
Denial pattern trends offer a comprehensive view of the reasons behind claim denials. By examining these trends, we can gain insights into systemic issues that might be affecting the billing process.
Common Denial Trends
Some common denial trends include:
- Coding Errors: Mistakes in coding are one of the most prevalent reasons for claim denials. Analyzing data can help identify specific codes that are frequently misused or incorrectly applied.
- Incomplete Information: Claims may be denied due to missing or incomplete information. Data analysis can reveal patterns in documentation errors that need to be addressed.
- Eligibility Issues: Denials related to patient eligibility can often be traced back to errors in verification processes. Identifying these patterns can help in refining eligibility checks.
By understanding these trends, healthcare providers can take proactive measures to address the root causes of denials, thereby improving their approval rates.
Analytics-Based Denial Prevention
Analytics-based denial prevention is a proactive approach that uses data insights to prevent claim denials before they occur. This strategy involves implementing changes based on the analysis of denial patterns and trends.
Steps to Implement Analytics-Based Denial Prevention
To effectively implement denial prevention strategies, consider the following steps:
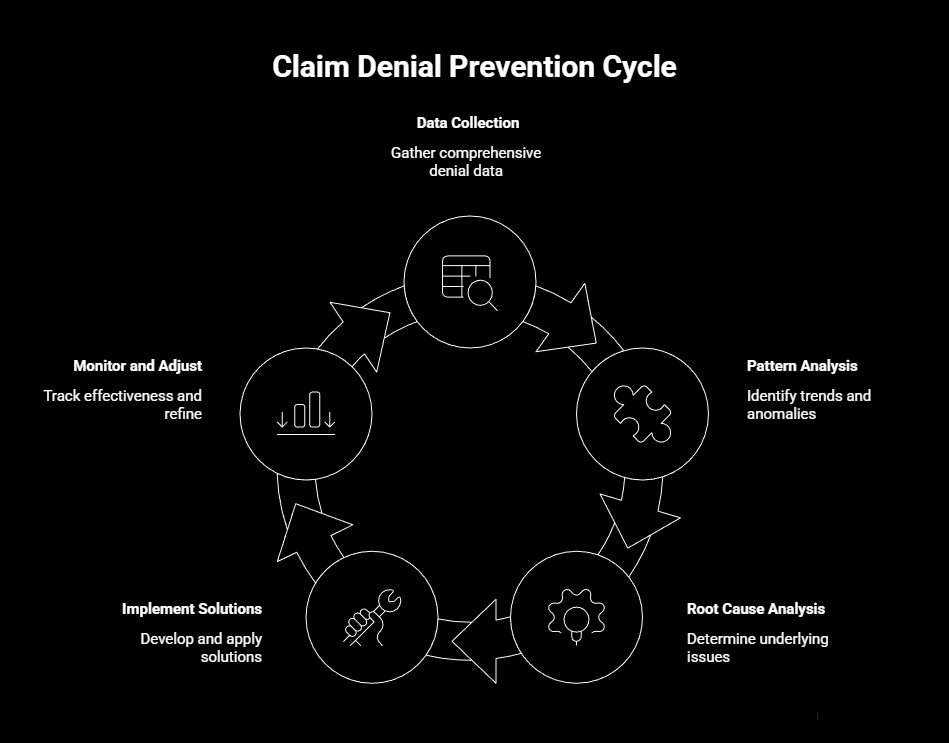
- Data Collection: Gather comprehensive data on all claim denials, including the reasons for denial, the departments involved, and any associated costs.
- Pattern Analysis: Use data analytics tools to identify patterns and trends in the collected data. Look for recurring issues that could indicate systemic problems.
- Root Cause Analysis: Once patterns are identified, conduct a thorough root cause analysis to determine the underlying issues contributing to claim denials.
- Implement Solutions: Develop and implement solutions based on the findings of the root cause analysis. This could involve staff training, system upgrades, or process changes.
- Monitor and Adjust: Continuously monitor the effectiveness of the implemented solutions and make adjustments as necessary to ensure ongoing improvement.
By following these steps, healthcare providers can significantly reduce the likelihood of claim denials, leading to improved financial performance and patient satisfaction.
The Role of Technology in Denial Prevention
Technology plays a crucial role in enhancing the effectiveness of denial prevention strategies. Advanced data analytics tools and software solutions can automate the process of identifying patterns and trends, making it easier for healthcare providers to implement effective denial prevention measures.
Key Technologies for Denial Prevention
Some key technologies that can aid in denial prevention include:
- Data Analytics Platforms: These platforms enable healthcare providers to analyze large volumes of data quickly and accurately, identifying trends and patterns that may not be immediately apparent.
- Machine Learning Algorithms: Machine learning can predict potential denial reasons by analyzing historical data, allowing providers to address issues proactively.
- Automated Verification Systems: These systems can streamline the eligibility verification process, reducing errors and improving claim approval rates.
By leveraging these technologies, healthcare providers can enhance their ability to diagnose and prevent claim denials, ultimately leading to more efficient and effective medical billing practices.
Claim denials are rarely isolated incidents—they’re patterns waiting to be identified. By leveraging claim denial analytics, tracking denial pattern trends, and implementing structured denial prevention strategies, we help healthcare providers move from reactive billing to proactive revenue protection.
At Pro MD Medical Billing, we use analytics-based denial prevention to diagnose the true root causes of denials and implement lasting solutions that strengthen the entire revenue cycle. When denial prevention is driven by data, providers don’t just recover revenue—they protect it before it’s ever at risk. Get in touch with us today to get started.