Understanding First-pass Claim Acceptance Rate (FPCR)
Every dollar a small medical practice loses to denied claims is a dollar that didn’t have to disappear. The first-pass claim acceptance rate — the percentage of claims a payer accepts and pays on the very first submission — is one of the most telling indicators of a billing operation’s health. According to industry benchmarks, top-performing practices consistently target a 95% threshold or higher. Falling short of that number triggers costly rework cycles, delayed reimbursements, and administrative drain that small practices can rarely afford. Understanding exactly what drives this metric is the essential first step — and the numbers tell a compelling story worth digging into.
Analyzing Current FPCR: Metrics and Benchmarks
Before improving your claim acceptance rate, you need a clear baseline. The industry benchmark most billing professionals reference is the 95% threshold — practices consistently achieving that or higher are operating efficiently. Those falling below it are losing meaningful revenue on every billing cycle.
Start by pulling denial reports from your clearinghouse and sorting rejections by reason code. Patterns reveal problems. A strong accounts receivable workflow makes this analysis far easier, turning raw data into actionable insight. Once you know where claims are failing, targeted improvements become straightforward.
Key Strategies to Boost First-pass Claim Acceptance Rate
Now that you have a baseline, it’s time to act on it. Improving medical billing claims performance isn’t about one silver bullet — it’s a layered approach where each fix compounds the last. According to best practices in revenue cycle management, the highest-performing practices consistently apply the same core disciplines: clean data, precise coding, proactive eligibility verification, and systematic error review. Accuracy at every touchpoint is the single most reliable driver of a stronger first-pass rate. Pairing these habits with revenue cycle automation can dramatically reduce manual entry errors before a claim ever leaves the practice. The sections ahead break each strategy down — starting with the foundational layer: patient data accuracy.
Optimizing Patient Data Accuracy
Patient data errors are one of the most preventable — and most costly — causes of claim rejections. In RCM first pass performance, accurate demographic and insurance information at the point of intake is non-negotiable. According to tips from revenue cycle experts, eligibility verification and correct patient data entry alone can dramatically reduce front-end denials. Verification of benefits before every visit — not just new patients — catches coverage changes, lapsed policies, and incorrect member IDs before a claim ever leaves your practice. The data you collect on day one either protects your revenue or undermines it.
Utilizing Technology for Claim Accuracy
The right billing software does more than automate submissions — it actively intercepts errors before they reach the payer. Claim scrubbing tools, integrated eligibility verification, and real-time coding alerts work together to drive meaningful claim denial reduction at the source. In practice, practices that invest in purpose-built RCM technology consistently see cleaner submissions across specialties — whether that’s a high-volume ENT practice or a complex endocrine caseload. According to Physicians Weekly, automated pre-submission claim edits are among the highest-impact steps a practice can take toward first-pass success. Technology doesn’t replace expertise — but it dramatically amplifies it. Of course, even the best tools only perform as well as the people running them, which is exactly why staff training becomes the next critical lever to pull.
Training Staff for Improved Billing Outcomes
Even the best claim scrubbing software can’t fully compensate for an undertrained billing team. Staff competency is a foundational driver of insurance claim acceptance — and in small practices, where one or two people often handle the entire revenue cycle, a single knowledge gap can ripple into consistent denials.
Effective training focuses on three areas: payer-specific rules, coding updates, and documentation standards. Payer requirements shift frequently, and staff who stay current through regular education cycles make far fewer submission errors. According to Physicians Weekly, clean claims start with teams that understand both clinical and administrative workflows — not just one or the other.
Consistent, structured training is what separates practices with 90% first-pass rates from those achieving 99%. Small practices that invest in even monthly billing huddles and annual coding updates see measurable improvements in submission quality.
The results of a well-trained team — working alongside optimized technology — are best illustrated by what happens in real practice settings, which the next section explores in depth.
Case Study: Small Practice Success in Improving FPCR
Consider a small, three-physician family practice struggling with a first-pass acceptance rate hovering around 78% — well below the industry benchmark of 95%. By systematically overhauling their revenue cycle management process — combining claim scrubbing tools, mandatory staff training, and weekly denial audits — they pushed that rate past 96% within six months. Reimbursements accelerated, administrative burden dropped, and cash flow stabilized noticeably. Practices that achieve consistent first-pass results demonstrate that structured, incremental improvements outperform reactive fixes every time. Of course, real-world results vary based on payer mix, specialty, and team capacity — but the underlying pattern holds. These gains don’t happen by accident; they come from closing specific, identifiable gaps. And that’s where many practices stumble — not from lack of effort, but from operating under persistent myths about what actually drives denials in the first place.
Common Misconceptions About First-pass Claim Denials
Many practices misdiagnose why their medical claims processing struggles persist. The biggest misconception? That denials are primarily caused by coding errors. In practice, eligibility issues, missing prior authorizations, and incorrect patient demographics collectively drive a larger share of first-pass failures than coding mistakes alone.
Another widespread myth is that higher claim volume naturally means lower acceptance rates. Small practices often assume size works against them — but a focused, well-trained team can consistently outperform larger, less disciplined billing departments.
A clean claim isn’t just about correct codes — it’s about submitting the right information, to the right payer, at the right time. Understanding where denials actually originate, rather than where practices assume they do, is what separates stagnant rates from sustainable improvement. Of course, even with accurate assumptions and strong processes, certain real-world constraints can still limit how quickly FPCR gains materialize.
Limitations and Considerations in FPCR Improvement
Even the most disciplined improvement efforts hit real-world friction. First-pass claim acceptance rate gains don’t happen overnight, and small practices should set realistic expectations. Staff turnover can erode hard-won process improvements quickly — training one biller doesn’t guarantee institutional knowledge sticks. Payer rule changes also move faster than most internal update cycles can track.
It’s worth acknowledging that chasing a perfect score isn’t always the goal. Sustainable, incremental progress — even moving from 82% to 90% — meaningfully impacts cash flow. Practices partnering with experienced billing specialists often accelerate this curve by leveraging expertise that’s difficult to build in-house. As the billing landscape continues evolving, so will the tools available to close these gaps — which brings us to one of the most exciting developments reshaping revenue cycle management today.
Future Trends: AI and the Evolution of Medical Billing
AI-powered claim scrubbing is rapidly shifting from a premium add-on to a baseline expectation. Intelligent billing platforms now flag coding mismatches, missing modifiers, and payer-specific rule violations before submission — dramatically reducing the manual review burden that strains small practices. For high-complexity specialties, interventional cardiology billing illustrates this shift clearly: automated precision on procedure-heavy claims protects reimbursement where manual oversight alone simply can’t keep pace.
Clean claims submitted faster, with fewer human touchpoints, is where billing is heading. Practices that adopt AI-assisted workflows now will build a compounding advantage — each clean claim cycle generates better denial pattern data, which further sharpens future submissions. The practices that embrace these tools earliest will find the key takeaways ahead far easier to implement in practice.
Key Takeaways
Improving first-pass claim acceptance rate isn’t a single fix — it’s a compound strategy. Clean eligibility verification, precise coding, and proactive claim scrubbing each reinforce the others. Small practices that benchmark consistently, train staff regularly, and embrace AI-assisted tools position themselves ahead of the curve. The 99% first-pass acceptance rate that top-performing billing operations achieve is attainable — but only through systematic, sustained effort across every touchpoint in the revenue cycle.
Understanding why claims fail is just as critical as knowing how to prevent rejections. With that in mind, let’s break down the most common denial categories hitting practices hardest right now.
What Are the Top 5 Denials in Medical Billing?
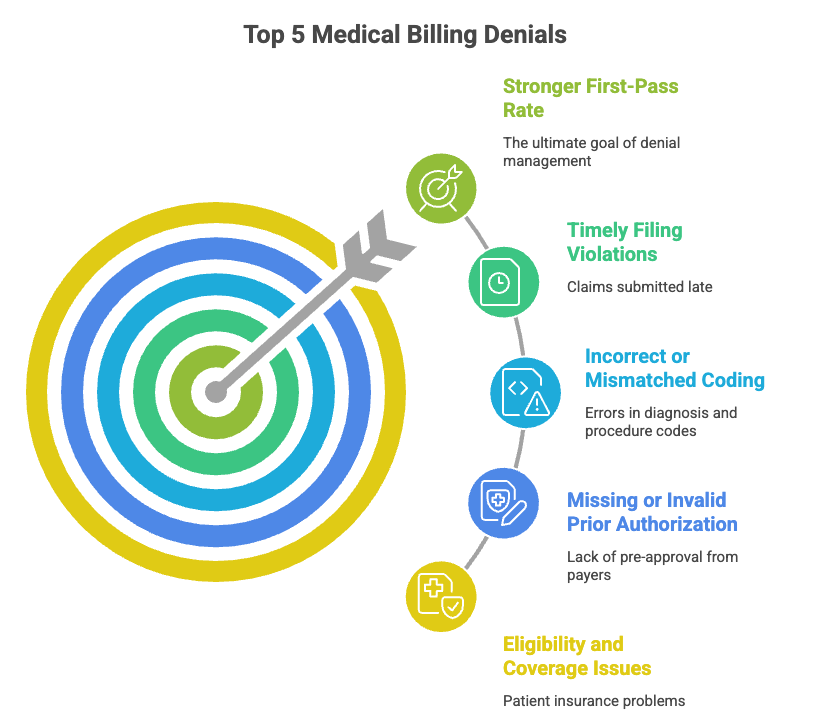
Understanding denial patterns is the foundation of a stronger first-pass rate. According to industry best practices, the five most common claim denials are:
- Eligibility and coverage issues — patient insurance is inactive or benefits don’t cover the service
- Duplicate claim submissions — the same claim filed twice triggers automatic rejection
- Missing or invalid prior authorization — payers require pre-approval that wasn’t obtained
- Incorrect or mismatched coding — diagnosis-to-procedure code mismatches and bundling errors
- Timely filing violations — claims submitted outside the payer’s deadline window
Each denial type is preventable. Practices that streamline their claims process through systematic front-end verification and coding audits consistently catch these issues before submission. Denial prevention, not denial management, is where small practices reclaim the most revenue. Knowing your top denial reasons by payer unlocks a targeted fix rather than a generic one.
ProMD Medical Billing
Small practices don’t need a massive billing department to achieve elite claim acceptance rates — they need the right partner. ProMD Medical Billing delivers a 99% first-pass claim acceptance rate, backed by structured workflows covering eligibility verification, coding accuracy, and real-time claim scrubbing. A clean claim submitted correctly the first time is always faster and cheaper than chasing a denial. For specialty-specific needs, practices can explore billing support built for complex cases to see how that standard translates across high-scrutiny service lines.
What Are the Top 5 Denials in Medical Billing?
Knowing your enemy is half the battle. The most common denial categories — eligibility issues, duplicate claims, missing or invalid codes, authorization failures, and timely filing violations — account for the vast majority of rejected revenue. Each one is preventable. Eligibility errors alone drive a significant share of front-end denials, which is why real-time verification before every visit is non-negotiable. Recognizing these patterns transforms your denial management from reactive firefighting into a proactive, systematic defense.
What Is the Highest Paid Medical Biller?
Compensation in medical billing scales directly with specialization and expertise. The highest paid medical billers typically work in complex specialties — think surgical subspecialties, oncology, or anesthesia — where coding nuance directly impacts revenue. Senior billing professionals with Certified Professional Biller (CPB) or Certified Medical Reimbursement Specialist (CMRS) credentials consistently command top salaries.
Specialized expertise is the single greatest salary differentiator in medical billing — generic skills plateau quickly, but specialty-specific mastery compounds in value. As AI continues reshaping the billing landscape, that expertise question is about to get a lot more complicated.
Are Medical Coders Going to Be Replaced by AI?
This question comes up constantly — and the honest answer is no, not entirely. AI is transforming medical coding by automating repetitive tasks and flagging potential errors, but human oversight remains irreplaceable. Complex diagnoses, payer-specific nuances, and compliance judgment calls still demand experienced coders. AI augments skilled coders rather than replacing them — and practices that embrace both will consistently produce cleaner claims. Speaking of clean claims getting paid quickly, the next critical factor is when payers are required to pay them.
What Is Prompt Pay in Medical Billing?
Prompt pay refers to state-mandated deadlines requiring insurers to process and pay clean claims within a specified timeframe — typically 30 to 45 days from receipt. For small practices, understanding prompt pay laws is a direct revenue protection strategy. When a clean claim sits unpaid beyond the statutory window, the insurer may owe interest penalties, giving practices legitimate leverage to recover delayed payments. That connection between clean claims and faster reimbursement is exactly why improving your first-pass acceptance rate matters so practically — a claim accepted on the first submission starts the prompt pay clock immediately.
What Do You Need to Do to Be a Private, Insurance-Friendly Practice?
Being insurance-friendly means your practice is structured to meet payer expectations at every touchpoint — from credentialing to claim submission. In practice, that means maintaining current provider enrollment, verifying patient eligibility before every visit, and using payer-specific code sets consistently.
Small practices that align their workflows with insurer requirements see fewer denials, faster reimbursements, and stronger patient trust. A clean, payer-aligned practice isn’t just operationally efficient — it’s a competitive advantage.
Partnering with a dedicated billing team can accelerate this alignment significantly.
How Can a Medical Billing Company in the USA Help Improve First-Pass Rates?
A specialized medical billing company brings the infrastructure, expertise, and payer intelligence that most small practices simply can’t build in-house. Clean claims don’t happen by accident — they’re the product of systematic processes applied consistently across every single submission.
In practice, a billing partner handles real-time eligibility verification, coding audits, and denial pattern analysis simultaneously — tasks that overwhelm solo billers. That operational depth translates directly into higher first-pass acceptance rates without adding headcount to your payroll.
For mid-sized groups weighing this decision, the return-on-investment question becomes especially compelling — and that’s exactly where the next section digs in.
Is It Worth It for a Mid-Sized Medical Group to Use RCM Services?
Absolutely — and the ROI case is compelling. Mid-sized groups face a compounding problem: claim volume is high enough that manual errors become costly at scale, yet margins are often too tight to staff a full in-house billing department. Revenue cycle management (RCM) services bridge that gap by delivering enterprise-grade infrastructure without enterprise-level overhead.
Clean claims don’t just save time — they protect every dollar your providers work to earn. Even marginal improvements in first-pass rates translate directly into faster cash flow and reduced write-offs across hundreds of monthly claims. That momentum compounds quickly, making denial management — which we’ll explore next — far less of a burden.
How Do Medical Billing and Coding Services Handle Denied Claims?
Professional billing and coding services don’t just submit claims — they build systematic denial management workflows that convert rejections into recovered revenue. When a claim is denied, a structured process kicks in: the denial is categorized by reason code, routed to a specialist, corrected, and resubmitted within payer-specific timelines.
Denied claims rarely signal a permanent loss — they signal a process gap that, once fixed, prevents the same error from recurring. That’s the operational mindset that separates reactive billing from truly optimized revenue cycle management. As practices scale, that distinction becomes everything.
What Reliable Medical Billing Services Are Available for Small Practices?
Small practices don’t have to navigate claim optimization alone. A strong medical billing partner delivers clean claims workflows, denial management, and real-time reporting — everything covered in this article, handled systematically. In practice, the right service combines credentialed coders, payer-specific rule libraries, and eligibility verification tools that drive first-pass rates consistently above 95%. That combination of expertise and technology is exactly why outsourcing has become the preferred path — and there are more compelling reasons to make that move than most practice owners realize.
What Are 10 Reasons to Outsource Medical Billing Services?
Building on the small-practice solutions discussed earlier, outsourcing takes those advantages even further. Outsourced medical billing consistently delivers results that in-house teams struggle to match:
- Higher first-pass rates through dedicated claim scrubbing expertise
- Reduced overhead — no salaries, benefits, or training costs
- Faster reimbursements from cleaner submissions
- Denial management workflows already built and tested
- Coding compliance updated continuously with regulation changes
- Scalability as patient volume fluctuates
- Real-time reporting and transparent performance dashboards
- Reduced administrative burden on clinical staff
- HIPAA-compliant infrastructure without internal IT investment
- Specialty-specific expertise across complex billing scenarios
Clean claims don’t happen by accident — they’re the product of purpose-built systems working consistently behind the scenes.
Choosing the right outsourcing partner, however, matters enormously. Not every vendor delivers equally on these promises.
What Is a Good Company for Outsourcing Medical Billing?
Choosing the right outsourcing partner is one of the highest-leverage decisions a small practice can make. The best companies combine specialty-specific coding expertise, transparent reporting, and a documented track record of high first-pass acceptance rates. Look for partners who publish clear performance benchmarks, offer dedicated account managers, and demonstrate payer-specific knowledge for your specialty. A strong outsourcing partner doesn’t just submit claims — they proactively identify workflow gaps before errors reach the payer. That distinction separates good vendors from great ones, and it’s exactly where denial patterns become the next critical conversation.
What Are the Top 5 Denials in Medical Billing?
Understanding denial patterns is what separates practices that consistently hit high first-pass rates from those stuck in rework cycles. The top five denials small practices encounter are: missing or invalid patient information, duplicate claim submissions, incorrect or unsupported diagnosis codes, lack of prior authorization, and non-covered services. Each one is preventable. Addressing these five root causes systematically—through eligibility checks, coding audits, and authorization workflows—builds the foundation every strong revenue cycle depends on.
ProMD Medical Billing
Improving your first-pass claim acceptance rate isn’t a one-time project — it’s an ongoing discipline built on clean data, smart workflows, and the right billing partner. From eligibility verification and accurate coding to denial pattern analysis and staff training, every strategy covered in this article compounds over time.
A practice that masters these fundamentals consistently captures revenue it would otherwise leave behind. Ready to stop chasing denials and start maximizing clean claims? The strategies are here — now it’s time to implement them.