The next wave of regulatory change is already taking shape, and the CMS 2026 updates are expected to significantly influence reimbursement models, Medicare billing rules, and overall CMS compliance expectations. For medical practices, upcoming reimbursement policy shifts can directly affect cash flow, audit exposure, and operational efficiency. Preparing early allows us to stay ahead of compliance risks while protecting revenue. At Pro MD Medical Billing, we work alongside practices to interpret CMS changes proactively and build billing strategies that support long-term financial stability instead of last-minute reaction.
Understanding what’s changing—and how those changes impact daily billing operations—puts practices in control well before new policies take effect.
Understanding the 2025 CMS Updates
Before taking action, we need a clear understanding of how the CMS 2026 updates build upon recent CMS policy direction. These changes continue CMS’s broader initiative to improve care quality, strengthen payment accuracy, and increase oversight tied to Medicare billing rules and documentation integrity. For providers, this means tighter scrutiny of claims, clearer justification of medical necessity, and greater emphasis on compliance workflows.
Key areas of focus include:
- Value-Based Care Models: Emphasizing outcomes over volume, these models aim to improve healthcare quality while controlling costs.
- Medicare Billing Rules: Adjustments to billing procedures will require practices to adapt to new coding and documentation requirements.
- CMS Compliance: Enhanced compliance measures will necessitate thorough understanding and implementation of new guidelines.
By familiarizing ourselves with these changes, we can better prepare our practices to adapt and thrive in the evolving healthcare landscape.
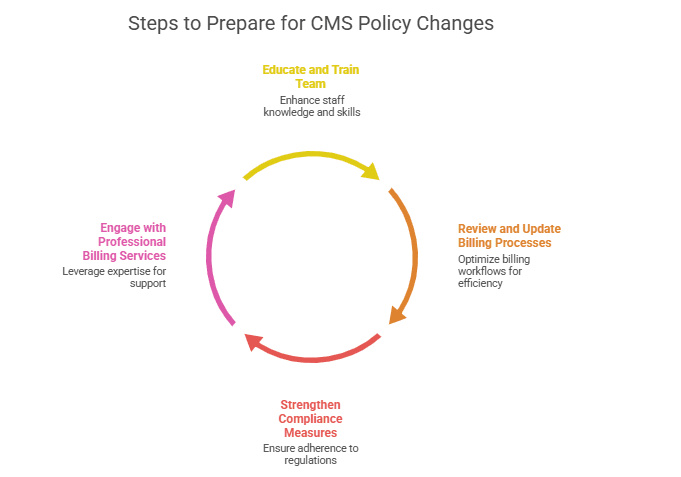
Steps to Prepare for CMS Policy Changes
1. Educate and Train Your Team
Staff education remains one of the strongest safeguards against revenue disruption. As Medicare billing rules evolve under the CMS 2026 updates, everyone involved in documentation, coding, and billing must be aligned. We recommend:
- Regular Training Sessions: Conduct ongoing training to keep staff updated on the latest billing codes and compliance requirements.
- Access to Resources: Provide access to CMS guidelines and educational materials to enhance understanding.
- Engagement with Professional Organizations: Encourage participation in workshops and seminars offered by professional healthcare organizations.
By investing in education, we empower our team to navigate changes confidently and maintain compliance with new regulations.
2. Review and Update Billing Processes
Policy changes often expose weaknesses in outdated billing workflows. Preparing for the CMS 2026 updates means taking a close look at how claims move from documentation to submission. Key steps include:
- Audit Current Practices: Conduct thorough audits of existing billing procedures to identify potential areas for improvement.
- Implement Technology Solutions: Leverage technology to automate billing processes, reducing errors and improving efficiency.
- Enhance Documentation Practices: Ensure that documentation is comprehensive and meets the requirements of the new CMS guidelines.
At Pro MD Medical Billing, we help practices refine these processes to improve clean claim rates and protect reimbursement.
3. Strengthen Compliance Measures
CMS compliance will be a major focal point under the 2026 policy changes. Practices that treat compliance as an ongoing process—not a one-time task—are far better positioned for long-term stability. Important actions include:
- Compliance Audits: Regularly conduct compliance audits to identify and address potential gaps.
- Policy Updates: Revise internal policies to align with the new CMS guidelines, ensuring that all staff are aware of the changes.
- Risk Management: Implement a comprehensive risk management strategy to mitigate potential compliance issues.
By prioritizing compliance, we can avoid penalties and maintain a positive reputation within the healthcare community.
4. Engage with Professional Billing Services
Navigating CMS changes internally can be resource-intensive. Partnering with experienced billing professionals provides both clarity and protection. Working with Pro MD Medical Billing allows practices to benefit from:
- Expertise and Experience: Leverage the expertise of professionals who are well-versed in CMS updates and compliance requirements.
- Customized Solutions: Receive tailored solutions that align with your practice’s unique needs and goals.
- Ongoing Support: Benefit from continuous support and guidance as new changes are implemented.
By collaborating with experienced billing services, we can streamline our operations and focus on delivering quality patient care.
Maintaining Revenue Streams Amidst Changes
Preparing for CMS 2026 updates isn’t only about compliance—it’s also about safeguarding revenue during periods of transition.
1. Diversify Revenue Sources
Diversifying revenue sources can provide a buffer against potential disruptions. Consider:
- Expanding Services: Offer additional services that align with patient needs and preferences.
- Exploring Telehealth Opportunities: Leverage telehealth to reach a broader patient base and enhance convenience.
- Participating in Value-Based Programs: Engage in value-based care programs that offer financial incentives for improved outcomes.
By diversifying our revenue streams, we can enhance financial resilience and reduce reliance on a single source of income.
2. Optimize Patient Engagement
Engaging patients effectively can lead to improved satisfaction and increased revenue. Strategies include:
- Patient Education: Educate patients about the value of preventive care and adherence to treatment plans.
- Enhanced Communication: Utilize digital tools to improve communication and facilitate appointment scheduling.
- Feedback Mechanisms: Implement feedback mechanisms to gather insights and make improvements based on patient input.
By prioritizing patient engagement, we can build strong relationships and foster loyalty, ultimately boosting revenue.
3. Monitor Financial Performance
Regularly monitoring financial performance is crucial to identify trends and make informed decisions. Key actions include:
- Financial Reporting: Utilize comprehensive financial reports to track revenue, expenses, and profitability.
- Benchmarking: Compare performance against industry benchmarks to identify areas for improvement.
- Cost Management: Implement cost management strategies to optimize resource allocation and reduce waste.
By staying informed about our financial performance, we can make strategic adjustments to maintain stability and growth.
The CMS 2026 updates bring meaningful change to reimbursement structures, Medicare billing rules, and CMS compliance expectations. By educating teams, strengthening billing workflows, reinforcing compliance programs, and partnering with experienced professionals, practices can navigate upcoming reimbursement policy shifts without sacrificing revenue.
At Pro MD Medical Billing, we help practices prepare strategically—not reactively—so they remain compliant, financially stable, and positioned for long-term success. As CMS continues to refine its policies, staying proactive is the most effective way to protect both revenue and peace of mind.
To learn how we support practices through evolving CMS requirements, contact Pro MD Medical Billing and start preparing today.